The difference and distinction between varicose veins and rheumatism: comparison and relationship
Rheumatoid arthritis is a disease that affects the joints while varicose veins are a vascular condition that impacts the veins in the legs.
Rheumatoid arthritis is a disease that affects the joints while varicose veins are a vascular condition that impacts the veins in the legs.
- What is Rheumatoid Arthritis
- Rheumatoid Arthritis Symptoms
- Rheumatoid Arthritis Causes
- Rheumatoid Arthritis Treatment Methods
- Varicose Vein Causes and How They Start
- Key Varicose Vein Symptoms
- Connection and Comparison Between Varicose Veins and Rheumatoid Arthritis
Rheumatoid arthritis and varicose veins are common conditions often confused due to similar symptoms like leg pain and discomfort. However they differ in origin symptoms causes and treatments. This article helps clarify these differences for better understanding. If unsure about your condition consult a specialist.
What is Rheumatoid Arthritis
Rheumatoid arthritis (RA) is an autoimmune disease where the immune system attacks joint tissues causing chronic inflammation pain swelling and stiffness. It typically affects small joints like fingers wrists and knees but can spread elsewhere.
Rheumatoid Arthritis Symptoms
Key symptoms include:
- Joint pain and swelling especially in hands wrists and knees
- Morning stiffness lasting over an hour
- Severe fatigue
- Loss of appetite
- Fever
- Numbness or tingling particularly in hands and feet
- Firm painless lumps under skin near joints
- Reduced joint movement range
Rheumatoid Arthritis Causes
The exact cause is unknown but research suggests genetic and environmental factors play roles. These include:
- Family history
- Certain infections or diseases (gout lupus streptococcal infections)
- Exposure to chemicals like asbestos or silica
- Gender (higher in women)
- Obesity and excess weight
- Aging
- Stress
- Smoking
- Poor diet
Rheumatoid Arthritis Treatment Methods
Treatments fall into three main categories:
- Medications: Nonsteroidal anti-inflammatory drugs like ibuprofen reduce pain and inflammation. Disease-modifying antirheumatic drugs like methotrexate prevent progression biologics target immune system and corticosteroids reduce severe inflammation as prescribed.
- Physical Therapy: Helps maintain joint range and strengthen surrounding muscles. Aerobic activities like cycling or walking and exercises like yoga or swimming improve mobility.
- Surgery: For severe chronic cases surgery repairs or replaces damaged joints like knee or hip replacements.
Lifestyle changes like maintaining weight, healthy diet, stress management, adequate sleep and beneficial exercises also help.
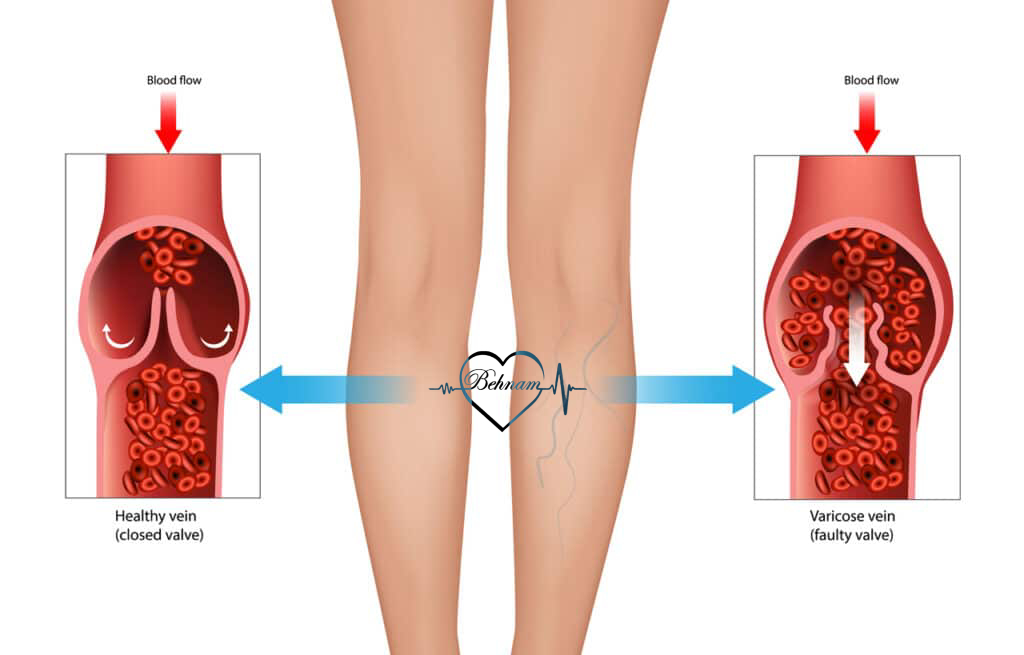
Varicose Vein Causes and How They Start
Varicose veins occur due to weakened vein walls or faulty valves acting as gates to control blood flow. Blood pools instead of returning to the heart causing vein swelling. Increased pressure enlarges and twists veins.
Key Varicose Vein Symptoms
Symptoms include:
- Leg heaviness pain or fatigue especially after prolonged standing
- Burning or throbbing sensations
- Swelling particularly in ankles or calves
- Itching around varicose veins
- Dry skin with red or brown discoloration
- Visible bulging twisted purple or dark blue veins
- Skin ulcers near ankles
- Bleeding and ulcer infections
Varicose Vein Causes and Risk Factors
Factors increasing risk include:
- Genetic and congenital factors
- Aging
- Pregnancy
- Prolonged standing or sitting
- Hormonal changes
- Gender (higher in women)
- Obesity and excess weight
- Sedentary lifestyle
- Unhealthy habits
If these risk factors apply finding a good varicose vein doctor or specialized clinic aids accurate diagnosis and effective treatment.
Varicose Vein Treatment Methods
Treatment methods for varicose veins include:
Preventive Methods: Lifestyle changes like regular exercise healthy diet, avoiding prolonged sitting or standing and weight control. Elevate legs for at least 15 minutes every few hours and use compression stockings as detailed in Varicose Vein Prevention Methods.
- Medical Treatments: Medications sclerotherapy (injecting sclerosant to collapse veins), laser therapy (surface or endovenous to seal faulty veins), and surgery for specific severe cases.
- Minimally Invasive Methods: Sclerotherapy (liquid or foam), endovenous treatments like EVLT (laser) or EVRF (radiofrequency), surface laser for small spider veins, phlebectomy (mini or micro), VenaSeal glue and venous endoscopy for deep veins.
Connection and Comparison Between Varicose Veins and Rheumatoid Arthritis
Research shows no direct link between varicose veins and rheumatoid arthritis but rheumatoid inflammation may pressure circulation indirectly contributing to varicose veins. Rheumatoid vasculitis a rare complication affects veins and may relate to varicose veins. However only 2-5% of rheumatoid patients develop varicose veins.
For clarity the table below shows differences and similarities between RA and varicose veins:
| Aspect | Rheumatoid Arthritis | Varicose Veins |
|---|---|---|
| Origin | Autoimmune joint attack | Vein wall or valve weakness |
| Symptoms | Joint pain, stiffness, fatigue, fever, numbness, lumps | Leg heaviness, burning, swelling, itching, discoloration, bulging veins, ulcers |
| Causes | Genetics, infections, chemicals, gender, obesity, aging, stress, smoking, poor diet | Genetics, aging, pregnancy, standing, hormonal changes, gender, obesity, sedentary, lifestyle |
| Treatments | Medications, physical therapy, surgery, lifestyle changes | Preventive methods, medications, sclerotherapy laser, surgery minimally invasive options |
Conclusion
Rheumatoid arthritis and varicose veins are distinct conditions with different causes symptoms and treatments. Rheumatoid arthritis is an autoimmune disease targeting joints with pain and stiffness. Varicose veins are vascular issues from blood pooling causing leg heaviness and visible veins. Consulting a specialist ensures proper diagnosis and treatment.
FAQs
Why do we get rheumatoid arthritis?
Genetics, immune dysfunction, aging, stress certain infections chemical exposure weight gain smoking and poor diet are key factors.
What is the most dangerous rheumatoid arthritis type?
Scleroderma, lupus, rheumatoid arthritis and rheumatoid vasculitis are most dangerous.
Does varicose veins have permanent treatment?
Yes, modern methods permanently remove affected veins but new ones may form without prevention.
What is rheumatoid arthritis' enemy?
Healthy weight diet, exercise, stress management, adequate sleep and quitting smoking combat rheumatoid arthritis.





