Why is heat not good for the varicose veins and what to do?
A common question from many patients with varicose veins is why their condition worsens in the heat and summer season. In this article we will examine the effects of heat on varicose veins and strategies to tackle it.

A common question from many patients with varicose veins is why their condition worsens in the heat and summer season. In this article we will examine the effects of heat on varicose veins and strategies to tackle it.
- How Heat Affects Varicose Veins
- Complications of Heat on Varicose Veins
- Types of Heat Exposure Affecting Varicose Veins
- Managing Varicose Vein Symptoms in Heat
The body reacts differently to cold and heat to adapt to its environment. The vascular system plays a key role in this adaptation. We explored cold’s effects on varicose veins in a previous article. This article examines how heat impacts varicose veins. Can heat therapy or warm compresses which soothe some pains help manage varicose vein symptoms? The answer is no.
What Causes Varicose Veins?
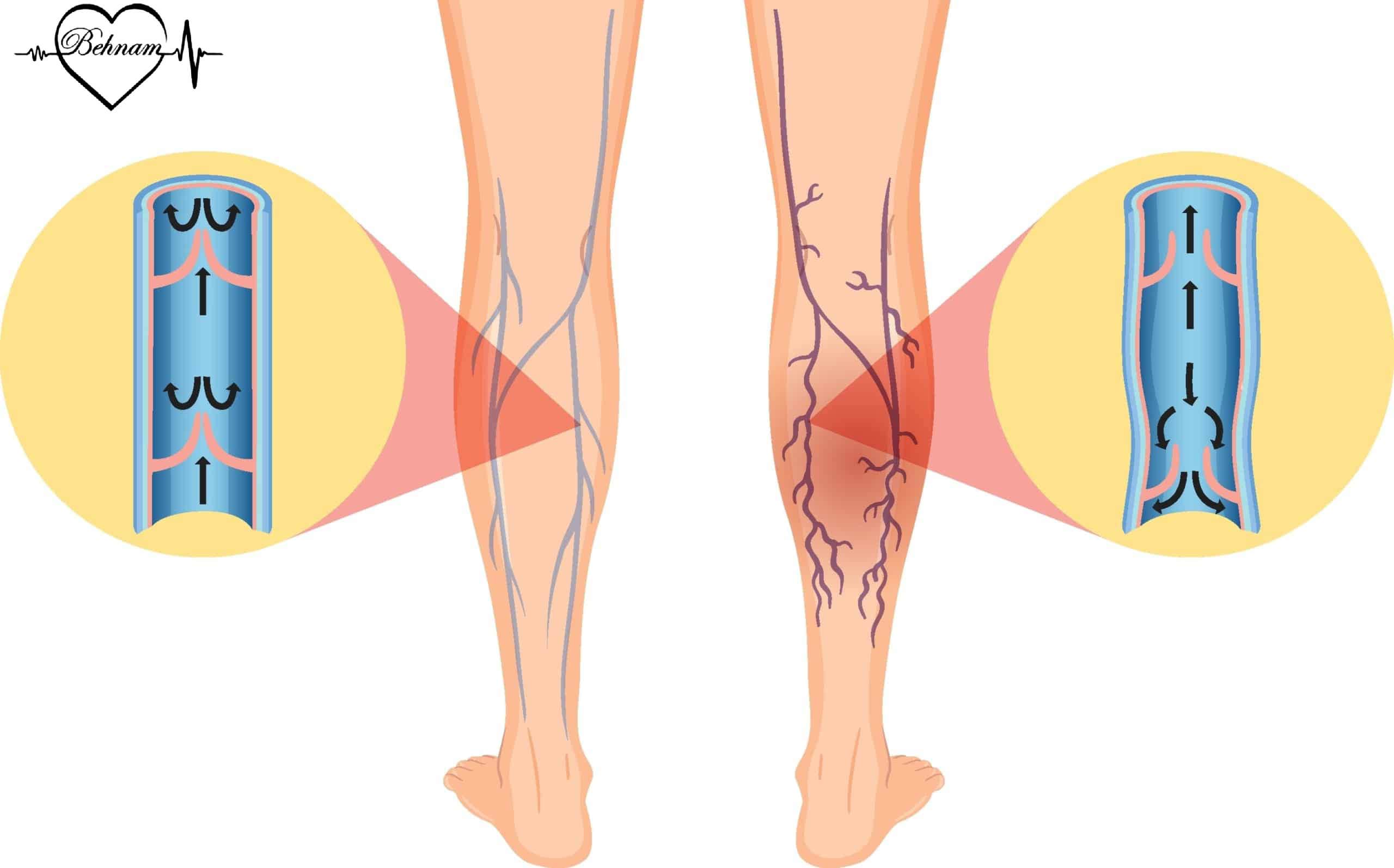
Varicose veins are swollen twisted veins often in the legs due to blood pooling. When vein walls or valves weaken blood fails to flow properly to the heart causing pressure and inflammation. Legs are more affected due to anatomy standing and gravity. Risk factors include genetics, obesity, prolonged sitting/standing, pregnancy, history of blood clots and low activity.
Varicose Vein Symptoms
Common symptoms include:
Heaviness and fatigue in legs
Muscle cramps especially in calves
Itching or tingling around varicose veins
Visible swollen twisted veins
Skin discoloration or dryness
Ulcers or bleeding
How Heat Affects Varicose Veins
When exposed to heat the body activates temperature regulation processes to prevent overheating. Blood vessels particularly near the skin dilate to increase blood flow and release heat. Superficial leg veins affected by varicose veins are more sensitive to temperature changes. Heat relaxes vein wall muscles increasing their diameter and slowing blood flow leading to more blood pooling in the legs.
Why Heat and Vein Dilation Are Problematic
Valve Dysfunction: Dilated veins aid temperature regulation but in varicose veins faulty valves worsen blood pooling increasing pressure on vein walls.
Increased Venous Pressure: Higher blood volume causes swelling heaviness and pain with a risk of vein rupture or bleeding.
Reduced Blood Flow: Heat slows blood flow increasing pooling especially in those standing long or in hot environments.
Complications of Heat on Varicose Veins
Swelling: Blood pooling in dilated veins causes swelling particularly in ankles and calves.
Pain and Heaviness: Increased pressure from blood buildup leads to fatigue and discomfort.
Severe Complications: Prolonged heat exposure in severe chronic varicose veins raises risks of vein rupture skin ulcers bleeding or blood clots.
Types of Heat Exposure Affecting Varicose Veins
Hot Baths or Swimming: Hot water increases body temperature and dilates veins worsening blood pooling and valve dysfunction. Use lukewarm water below 37°C for bathing or swimming.
Sauna or Hot Tub: High humidity in saunas or hot tubs stimulates skin blood flow and may increase venous inflammation. Avoid them if you have varicose veins.
Summer Heat: Prolonged sun exposure or hot climates increases skin blood flow reducing venous return causing swelling and heaviness. Sunlight may also damage varicose areas. Use hats sunscreen and cool legs regularly.
Intense Heating Devices in Winter: Heaters can raise room temperatures significantly mimicking summer heat effects. Maintain room temperatures between 20-22°C with proper ventilation.
Warm Compresses or Heat Therapy: Heat pads or hot water bottles used for muscle pain worsen swelling and inflammation. Use cold compresses instead.
Infrared Radiation: Devices using infrared waves create deep tissue heat increasing vein swelling and discomfort. Avoid for varicose veins or consult a doctor.
Managing Varicose Vein Symptoms in Heat
To reduce symptoms in hot weather:
Keep Cool: Cool your body and legs regularly using cold compresses or water.
Wear Compression Stockings: They prevent excessive vein dilation and improve venous return. Consult a doctor for the right type and class.
Elevate Legs: Raise legs above heart level for at least 10 minutes multiple times daily to reduce gravity’s pressure and aid blood flow.
Stay Hydrated: Drink enough water to avoid dehydration which worsens vein dilation and heat-related issues. Use sugar-free electrolyte drinks during activity.
Healthy Diet: Eat fiber-rich fruits vegetables and low-salt foods avoiding processed or fatty foods to support vascular health.
Wear Loose Clothing: Tight clothes like pants belts or shoes strain veins. Choose loose breathable clothing especially in heat.
Limit Heat Exposure: Avoid prolonged heat or sun exposure. Be active in cooler times like early morning or evening. Use hats and sunscreen.
Cold Water Therapy: Apply cold water or compresses for 10-15 minutes to constrict veins reduce swelling and pain. Adding Epsom salt (magnesium) may help. Avoid using ice or cold water for over 20 minutes or if you have ulcers bleeding or infections; consult a doctor.
Avoid Intense Activity: Heavy exercise in heat combines physical strain and heat effects increasing blood flow to the skin and reducing venous return. Avoid strenuous activities like running or heavy labor in hot conditions.
Treating Varicose Veins
For severe or chronic varicose veins consider definitive treatments before heat or other factors worsen symptoms. Modern treatments are less invasive than in the past. Learn more in Varicose Vein Treatments.
Conclusion
Vein dilation from heat is a natural response to regulate body temperature but in varicose veins it exacerbates blood pooling venous pressure swelling and pain due to faulty vein walls and valves. Preventive measures symptom management and medical consultation for severe cases are essential.
FAQs
Can heat worsen my varicose veins?
Yes heat dilates veins and with faulty valves in varicose veins it increases blood pooling pressure swelling inflammation and pain.
Can I exercise in summer with varicose veins?
Exercise in summer is not harmful but choose cooler times avoid heavy activities elevate legs stay hydrated and wear compression stockings.
Is using a heating pad or hot water bottle helpful for varicose vein pain?
No heat pads or hot water bottles worsen swelling and pain. Use cold compresses, leg elevation and compression stockings for relief.
Can heat cause varicose vein rupture or bleeding?
In rare cases intense heat like saunas or hot baths can increase venous pressure causing rupture or bleeding especially in advanced chronic varicose veins near the skin.





